Anesthesiology is one of the most detail-driven specialties in modern healthcare, where providers are responsible for patient safety from pre-operative evaluation through intraoperative monitoring and post-anesthesia recovery. Every minute matters not only clinically but also financially, which is why specialized anesthesia medical billing services are essential. Unlike most specialties that rely on standard CPT fee schedules, anesthesia reimbursement requires precise calculation of base units, time units, physical status modifiers, and payer-specific conversion factors, and even small documentation gaps can result in denials, underpayments, or compliance risks.
At PMBS, the focus is on optimizing anesthesia revenue cycles so providers are paid accurately and on time. Anesthesia billing follows a unique formula in which base units, time units, and modifiers are combined and multiplied by a conversion factor, making accurate start and stop times, compliant medical direction documentation, correct physical status modifiers, and strict adherence to payer rules critical for full reimbursement. Anesthesia care teams often include anesthesiologists, Certified Registered Nurse Anesthetists, and anesthesiologist assistants, each with distinct billing requirements, particularly in cases involving medical direction or supervision, where incorrect use of modifiers such as QK, QX, QY, QZ, or AA can significantly reduce payment.
Comprehensive anesthesia billing support covers the entire revenue cycle, including eligibility and benefits verification, CPT, ASA, and ICD-10 coding, time unit validation, modifier accuracy checks, clean claim submission, denial management, underpayment recovery, accounts receivable follow-up, and compliance monitoring. By addressing common issues such as inaccurate time documentation, missing medical direction attestations, improper physical status reporting, conversion factor errors, and delayed follow-up, specialized billing processes help eliminate revenue leakage before claims are submitted rather than after denials occur.
Explore how our medical billing services also support Cardiology practices.
We understand the unique requirements of anesthesia billing and practice management and the challenges practitioners face while billing operations. Errors in medical billing have a massive impact on reimbursements. We provide customized medical billing solutions to optimize your anesthesia revenue cycle. We have already provided all medical billing services to providers with multiple specialties, and we can easily configure their needs and complexities. We can give you peace of mind while managing interconnected patient scheduling, anesthesia coding & billing, and invoicing. Anesthesia billing can be a hassle for new anesthesiologists as it demands proper documentation of a high number of records, such as:
The pre-surgery Consultation includes the examination of a patient and their family's medical history. In this procedure, an anesthesia specialist checks the drugs or tobacco habits the patient or anyone in its parents have. This has to be considered while calculating the required dosage of anesthesia medicines.
An anesthesia sheet involves the thorough documentation of the following aspects:
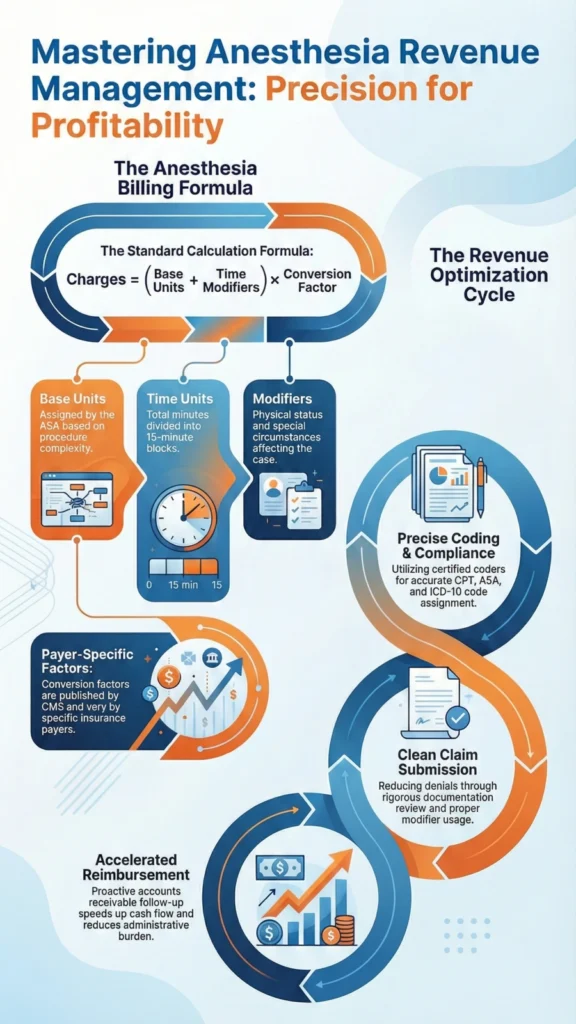
Base Units: The base units show the skills, certifications, and complexities required for the anesthetic service provided.
Time Units: Time units show the total Time spent with the patient while facilitating and administering the anesthetic medicines. These units also include the Time spent monitoring the patient's condition before, during, and after the surgery. The formula for calculating total time units is the total minutes of services divided by 15.
Modifiers such as (-AA, -QK, -QY, -QZ, and -QX) explain the role of anesthesia, and CRNA provides a means by which a service can be altered without changing the procedure code. They provide a platform by which anesthesia services can be catered to without any amendments to the procedure code. These modifiers add more information to the process. Besides this, they play a crucial role in unbundling and duplicating the billing process as an additional benefit. Modifiers are also used to enhance code consistency, capture payment data, and ensure reimbursement accuracy. In anesthesia, every anesthesia procedure billed to Medicare must include one of the following anesthesia HCPCS modifiers:
AA: Anesthesia services personally performed by an anesthesiologist. This modifier allows full fee schedule reimbursement.
AD: Medical supervision by an anesthesiologist: more than 4 concurrent anesthesia procedures.
The anesthesia pricing modifiers shall be listed first to ensure correct reimbursement.
The formula for calculating the Anesthesia reimbursement is (Base Units + Time Units + Modifiers) x Conversion Factor = Anesthesia Reimbursement.
Avoid billing for the following procedures; they shouldn't be merged with anaesthesia procedures. These are other particular procedures. Do not bill for the Injection of diagnostic or therapeutic substances along with anesthesia procedures (62320 – 62321 and 62324 – 62325)
Nerve Blocks (64400 – 64530)
Transesophageal Echo (TEE) (93312 – 93318)
Laryngoscopy (31505, 31515, 31527)
Bronchoscopy (31622, 31645, 31646)
The post-operative review comprises the records that state the success of an anesthesiology service primarily while depending on its ability to generate & collect revenue.
Successful and applicable anesthesia medical billing strategies include a proficient and trained revenue cycle managing team that can provide enhanced specialty-specific billing services with the assurance of compliance with regulations and protocols. Premium Medical Billing Solutions has a dedicated team of expert billers and coders who have served providers in the USA for ten years. We can provide you with optimum anesthesia billing services to grow your practice.
We are obtaining authorization and validating the patient’s eligibility and benefits before the surgery. We also know the services that can or cannot be bundled with the anesthesiology service offered. In case of the absence of a valid medical reason for the necessity of a drug administered, we follow up with the physician, clarify the medical necessity for the procedure, and state it clearly to claim rejection. Our expertise in Anesthesiology billing & coding includes but is not limited to:
By obtaining prior authorization and verifying the patient’s eligibility and benefits before the surgery, we can kill 60% of the chances of denials at the start. We also provide services to the providers, where we know all the facilities and treatments that can or cannot be bundled with the healthcare services offered by anesthesiologists. Our expertise in anesthesiology billing services also includes the following:
Topical INfiltration refers to the dosage of local anesthesia drug injected directly into body tissues, specifically at the area where there is a wound or requires a surgical procedure. This method is applied to numb the affected body so the patient can have painless surgery. Topical INfiltration required brilliant medical billing services, including accurate coding, claim submission, patient demographics, prior authorization, compliance with regulatory laws, and revenue cycle management. These services must be tailored according to the practice's needs and requirements.
Local anesthesia is used in minor surgeries, diagnostics, and dental procedures. This anesthesia involves the Injection of anesthetic drugs to numb a specific body area or part by blocking the nerve signals of the targeted body area. Medical billing services for local anesthesia practice include accurate coding, compliance, denial management, and claim submission. It also demands surety about proper documentation of the facilities that providers have provided to the patient, along with optimal credentialing of providers and revenue cycle management.
Metacarpal or digital blocks or metatarsal are precise local anesthesia. These are used to numb specific regions of feet, hands, or digits to perform painless surgeries on patients. Medical billing services for local anesthesia practices required accurate coding, claim submission, and compliance with payer regulations. Proper documentation, credentialing, and revenue cycle management are crucial to ensure efficient billing and reimbursement for metacarpal procedures. Our company has this expertise, and we provide seamless operations and financial outcomes in metacarpal anesthesia practices.
Anesthesia billing is based on time units and modifiers, not fixed CPT rates, and requires precise start and stop time documentation.
Time units are calculated by dividing total anesthesia time into 15-minute increments, starting with patient preparation and ending at anesthesia handoff.
Key modifiers include AA, QK, QX, QY, and QZ. Incorrect modifier usage can result in reduced payments or claim denials.
Common causes include incorrect time reporting, missing modifiers, and payer-specific anesthesia billing rules.
Yes. Anesthesia billing experts identify underpayments, correct claims, and appeal denials to recover lost revenue.
Copyright © 2026 Premium Medical Billing Solutions LLC. All rights reserved.